Updated: 11/7/23
If you’re looking for relief from the pain associated with porphyria, you’ve come to the right place! Porphyria is a complex group of disorders caused by an accumulation of chemicals called porphyrins or their precursors in the body. This can lead to abdominal pain and numbness, as well anxiety and insomnia – but it doesn’t have to be this way. In this blog post, we’ll explore various treatments and supplements that may provide some effective relief from symptoms caused by porphyria; everything from dietary changes to herbs and home remedies for managing your symptoms. Keep reading on if you’re ready to take back control over your health!
What is Porphyria?
Porphyria is the general name given to a group of disorders that arise when there’s a problem with the body’s ability to produce a chemical called heme. Heme is a major part of hemoglobin, the molecule found in red blood cells that carries oxygen to tissues in the body. The body makes heme in an eight-step process and each step relies on the action of a different enzyme. If one enzyme isn’t available, the process stops. This, in turn, causes a buildup of substances called porphyrins.
High levels of porphyrins can be toxic, leading to porphyria. The type of porphyria a person has depends on which enzyme is on short demand and therefore which type of porphyrin builds up. Some people never have symptoms while others have life-threatening episodes.
Most often, porphyria affects either the skin or the nervous system. Some types are more common among certain populations due to genetics. However, one form tends to occur as a result of lifestyle factors. There’s currently no cure for this rare group of conditions, but some treatments and therapies can help manage it.
Types of Porphyria and Symptoms
Researchers identified at least eight different types of porphyria. Some are more common than others, though all are considered rare. What makes this condition seem even less common is the fact that many people who have it never actually show symptoms.
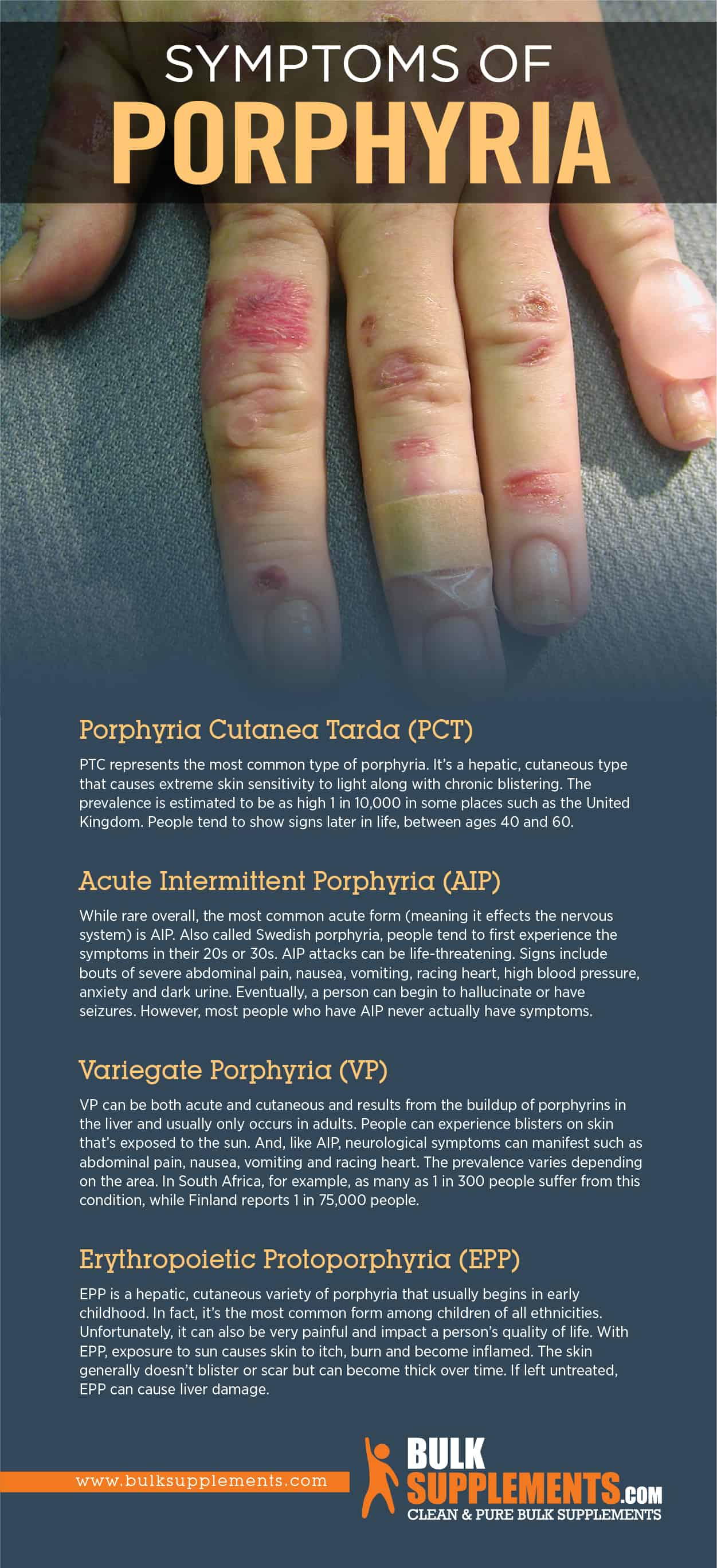
Acute Intermittent Porphyria (AIP)
AIP is the most common form of porphyria. It can cause a variety of symptoms, including abdominal pain, muscle pain, and visual disturbances. AIP is also associated with psychiatric symptoms including psychosis, depression, and anxiety.
Hereditary Coproporphyria (HCP)
Symptoms of HCP can range from mild to severe, and include abdominal pain, muscle pain, and neuropsychiatric symptoms, including psychosis.
Variegate Porphyria (VP)
VP is characterized by skin symptoms including blistering, scarring, and increased hair growth. The disorder can also cause respiratory problems, muscle weakness, and cognitive issues.
Congenital Erythropoietic Porphyria (CEP)
CEP is also called Günther disease. Symptoms include extreme photosensitivity, blisters on sun-exposed skin, anemia, and enlarged spleen.
Erythropoietic Protoporphyria (EPP)
EPP causes extreme photosensitivity, with the skin reacting severely to ultraviolet (UV) light. The disorder can also cause liver damage and increase the risk of liver cancer.
Hepatoerythropoietic Porphyria (HEP)
HEP is a rare form of porphyria that can cause abdominal pain, skin blisters, liver damage, and increased risk of liver cancer. Symptoms resemble those of AIP, but are less severe.
Porphyria Cutanea Tarda (PCT)
PCT causes skin problems, including blisters, scarring, and increased hair growth. The disorder is also associated with liver damage and increased risk of liver cancer.
ALAD-Deficient Porphyria (ADP)
ADP is a rare form of porphyria that causes abdominal pain, skin rashes, and increased risk of liver cancer. Symptoms can be managed with lifestyle changes such as avoiding alcohol and protecting the skin from UV light.
Symptoms of Porphryia
Abdominal Pain
For people with porphryia, abdominal pain is one of the most common symptoms and usually appears in the lower stomach region. The pain is often sudden, severe, and debilitating, and may last for several days. It can be accompanied by nausea, vomiting, and constipation. The pain is caused by the accumulation of heme precursors in the liver and other organs, leading to inflammation and damage.
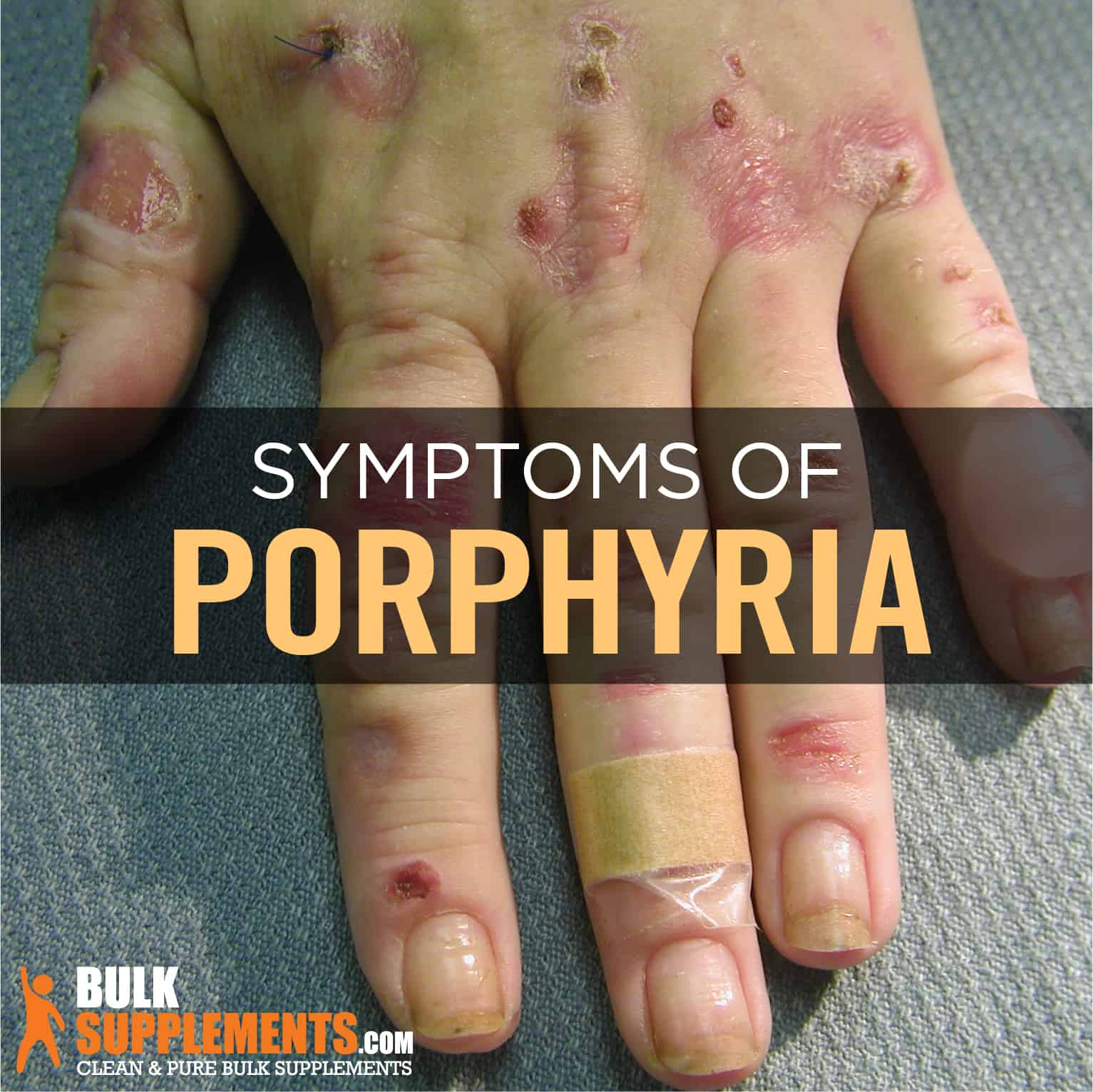
Skin Sensitivity
Another common symptom of porphryia is the increased sensitivity of the skin. The skin may become rashy, red, and easily damaged by minor injuries, sunlight exposure, and chemicals. If the condition becomes severe, patients may develop blisters, scarring, and pigmentation.
Oversensitivity to Sunlight
Individuals with porphryia can experience severe skin reactions and even blisters when exposed to sunlight. This condition referred to as photosensitivity, can make it difficult to carry out everyday tasks and affect an individual’s quality of life. While avoiding sunlight is a solution, it’s not practical, and medical advice should be sough
Fatigue
Porphryia can cause fatigue, which can affect a person’s ability to perform daily tasks. Some individuals might feel lethargic or have difficulty concentrating. The cause of this fatigue is not entirely understood, but it might be related to the buildup of porphyrins in the body.
Seizures
Seizures are a common symptom of acute intermittent porphryia (AIP), which is caused by an enzyme deficiency. Individuals with AIP experience seizures that can last up to several minutes and can be extremely dangerous. If you or a loved one is experiencing seizures, seek immediate medical attention.
Muscle Weakness
Another symptom is muscle weakness. Individuals with this condition experience sudden weakness or paralysis that typically affects the shoulders, arms, and legs. This symptom can be scary, particularly if it’s sudden. Nevertheless, it is essential to seek medical advice promptly.t.
Mood Disorders
Porphryia can likewise affect an individual’s mental health. Depression, anxiety, and other mood disorders have been reported in patients with porphryia. This could be because it can be challenging and confusing to live with such a rare disorder. It’s essential to make use of psychosocial support from family and friends and speak to your doctor if you experience any mental health symptoms.
Abnormal Hair Growth
One of the more unusual symptoms of porphryia is hair growth on unusual parts of the body. If you are experiencing hair growth in places you don’t normally, such as your cheeks, chin, or forehead, it could be a sign of porphryia. Additionally, if you are experiencing any pain or sensitivity around your joints, muscles, or wrists, it’s important to tell your doctor about it, as it can also be a sign of porphryia.
Breathing Difficulties
In severe cases, porphryia can lead to respiratory failure, leading to breathing difficulties. The buildup of porphyrins in the lungs damages the air sacs and reduces lung function, leading to shortness of breath and difficulty breathing. If you experience any breathing difficulties or shortness of breath, seek medical attention immediately.
Irregularities During Menstrual Cycle
For women, porphyria can cause irregular periods, intense pain during menstrual cycle and other hormonal disturbances.
Urinary Issues
Since porphyria affects the nervous system and energy metabolism, there can be urinary issues. These may include an abnormal amount of urine produced and urine that is the wrong color, which can mean that some of the byproducts are excreted out as opposed to being processed in the liver as they should be.
Causes of Porphyria
By understanding the causes and triggers of porphyria, as well as the symptoms, you can take steps to manage the condition and prevent attacks. Remember, with the right care and attention, it is possible to lead a healthy, active life with porphyria.
Genetics
The condition is usually caused by genetic mutations inherited from one or both parents, which affect the enzymes responsible for the synthesis of heme. Accordingly, some individuals diagnosed with porphyria may have a family history of the condition. In some rare cases, however, the mutations may occur spontaneously and without any known family history.
Hormonal Imbalance
A sudden disruption in hormonal levels can also trigger or aggravate the condition. This includes menstruation, pregnancy, and the use of contraceptives and hormonal therapies. It’s therefore essential to consult your health care provider before using any new medication that may affect your hormonal levels.
Environmental Factors
Certain environmental triggers can also activate the enzymes involved in porphyrin production leading to a porphyria crisis. These may include sunlight, dietary changes, infections, and chemicals such as alcohol, some drugs, and other toxins. In managing porphyria, it’s important to avoid situations or substances that may trigger a crisis. Your health care provider can help you identify and avoid potential triggers.
Sunlight Exposure
Patients with porphyria cutanea tarda are sensitive to sunlight and can develop skin rashes, blisters, and other skin problems when exposed to the sun. It’s crucial for patients to take measures to protect their skin from the sun, such as wearing protective clothing and applying sunscreen regularly.
Infection or Illness
In some cases, porphyria can be triggered by an infection or illness. For example, hepatitis C infection can trigger the onset of porphyria cutanea tarda. Patients with porphyria should take steps to prevent infection and manage their underlying health conditions to reduce the risk of developing symptoms.
Diagnosing Porphyria
Diagnosing porphyria can be challenging because the symptoms can mimic other conditions. The first step in diagnosing porphyria is to take a detailed medical history and perform a physical exam to look for signs of skin sensitivity, abdominal pain, and muscle weakness. If your doctor suspects that you may have porphyria, they may recommend blood or urine tests to look for porphyrins, the by-products of heme production. Genetic testing can also look for the specific genetic mutations that cause porphyria.
Treatment for Porphyria
There is no cure for porphyria, but there are often ways to manage it through diet, lifestyle and medication. Methods used to manage it depends on the type of porphyria. While diagnosis and prognosis of this condition is improving, even doctors still have a hard time properly identifying and managing it. As a result, few at-home proven remedies exist at this time.
Managing Symptoms and Preventing Attacks
Treatment for porphyria typically involves managing the symptoms and preventing attacks. Depending on the type of porphyria that you have, you may require regular blood transfusions to replace the missing enzymes that are responsible for producing heme. Other treatment options may include intravenous glucose to suppress the production of heme, medication to manage symptoms such as pain and nausea, and lifestyle modifications to help reduce stress triggers.
Medication
One of the main treatments for porphyria is medication. The medication given will vary depending on the type of porphyria a patient has. Patients with cutaneous porphyria may be prescribed chloroquine or a beta-carotene supplement. These medications help improve skin symptoms, such as skin blisters, swelling, and itching. Patients with acute porphyria, on the other hand, may be given intravenous glucose to support their blood sugar levels and prevent attacks.
Phlebotomy
Phlebotomy is a type of treatment that involves the removal of blood from the body. This treatment is particularly useful in patients with porphyria cutanea tarda (PCT), a condition that causes the liver to produce too much iron. By removing a unit of blood, the iron level has a reduction, and the symptoms of PCT alleviates.
Gene Therapy
One of the latest breakthroughs in porphyria treatment is gene therapy. Gene therapy is a type of treatment that involves introducing new genes into the body to replace missing or faulty genes. The aim of gene therapy is to correct genetic disorders at the molecular level, providing a long-term cure for the disease. In the case of porphyria, gene therapy involves introducing a new version of the defective gene that is responsible for producing heme. Although gene therapy is still in its early stages, it shows promising results in clinical trials, and it has an expectation to become widely available in the near future.
Stem Cell Transplantation
Another promising treatment for porphyria is stem cell transplantation. Stem cell treatment involves taking stem cells from the patient’s blood or bone marrow and transplanting them back into the patient after modification to produce the missing enzymes. This procedure not only replaces the missing enzymes but also provides a new source for making red blood cells. Although stem cell transplantation is a more invasive treatment option, it shows positive results in clinical trials and has an expectation to become widely available in the near future.
Hematin Infusion
Hematin infusion is an effective treatment option for acute intermittent porphyria. It is from human blood, and it can help to reduce the production of porphyrins. Hematin has intravenous infusion into the body over three to four days, and it significantly reduces the onset of acute attacks for individuals living with Porphyria.
Bone Marrow Transplantation
Bone marrow transplantation is another effective treatment option for porphyria. In this procedure, healthy bone marrow from a suitable donor experiences transplantation into the patient’s body. This transplant corrects the metabolic disorder that causes porphyria in the first place.
Sun Protection
One of the most common symptoms of porphyria is sensitivity to sunlight. Patients with cutaneous porphyria can protect their skin from the sun by wearing protective clothing and applying sunscreen with a high SPF.
Beta-Carotene
Beta-carotene is a plant pigment that experiences conversion into vitamin A in the body. It’s a powerful antioxidant that can help protect the skin from damage and reduce inflammation throughout the body. According to a study published in the Journal of the European Academy of Dermatology and Venereology, beta-carotene supplementation can help reduce the severity of porphyria-related skin damage.
Managing Porphyria
There is no cure for porphyria. However, lifestyle changes and medication can help manage the symptoms. One of the most critical aspects of managing porphyria is avoiding triggers. Triggers are anything that can exacerbate porphyria symptoms. For example, alcohol, certain medications, and stress can be triggers. It’s essential to identify your triggers and avoid them whenever possible.
Managing porphyria also involves a focus on overall good health. This includes maintaining a healthy diet and staying hydrated. It’s crucial to eat a balanced diet that includes plenty of fruits, vegetables and lean protein sources. Staying hydrated is also key to keeping porphyria symptoms at bay. Additionally, regular exercise can help improve overall health and reduce stress, which can be a trigger for some people.
To avoid sun exposure, it’s important always to wear protective clothing and to use sunscreen with a high SPF. Patients should also take care to manage their stress levels. Stress can trigger Porphyria symptoms, so it’s important to adopt stress management techniques like yoga, meditation, or breathing exercises.
Support groups can be incredibly helpful for patients with porphyria. Talking with others who are dealing with the same condition can provide much-needed support and comfort. There are also online resources that can provide information and support.
Diet for Porphyria
We’ll take a look at some of the specific foods and nutrients you should be incorporating into your diet, as well as those you should be avoiding.
Foods to Limit or Avoid
Foods high in porphyrins, such as red meat, shellfish, and organ meats, should generally be avoided by people with porphyria. Additionally, certain foods – including alcohol, caffeine, and artificial sweeteners – can trigger attacks by disrupting the production of heme in the liver. While everyone’s tolerance levels are different, it’s important to be aware of these potential triggers and avoid them if possible.
Nutrients to Focus on
Living with porphyria can also increase your risk of developing nutritional deficiencies, particularly in iron and B vitamins. B vitamins are critical for the production of heme in the liver, and iron plays an important role in the formation of red blood cells. Incorporating foods high in these nutrients – such as leafy greens, legumes, nuts, and fortified cereals – is key for managing symptoms and improving overall health.
Importance of Hydration:
In addition to nutrient intake, staying hydrated is essential for people living with porphyria. Dehydration can worsen symptoms and potentially trigger an attack, so it’s important to drink plenty of fluids throughout the day. Avoid sugary drinks and opt for water, herbal tea, or coconut water instead.
How Rare is Porphyria?
It’s quite rare. According to the National Organization for Rare Disorders (NORD), it affects approximately 1 in 20,000 people in the United States. This means that there are only around 6,000 people in the country who are affected by porphyria.
Porphyria and Vampires
Porphyria does not turn people into vampires. The connection between the two started in the 1980s when Dr. David Dolphin, a porphyria expert, suggested that some of the traits associated with porphyria, like sensitivity to sunlight and garlic, could have contributed to the vampire legend. However, there is no concrete evidence to prove this theory. Moreover, porphyria is not contagious, and people with porphyria are not harmful to others.
While porphyria patients do experience photosensitivity, their reaction to sunlight and other sources of light is very different from what is depicted in vampire movies and books. Sunlight exposure triggers an inflammatory response in the skin of porphyria patients, leading to pain, swelling and redness. Patients can avoid these symptoms by covering their skin or by using sunscreen with a high SPF. In contrast, vampires in popular culture burst into flames when they come into contact with sunlight, which is not a symptom of porphyria.
Porphyria is not the only medical condition that shares some similarities with the vampire legend. For example, there is a rare condition called erythropoietic protoporphyria (EPP), which also causes photosensitivity, but without the other symptoms of porphyria. EPP patients may also experience itching and burning sensations on their skin during exposure to sunlight. However, there is no need to associate EPP or any other condition with vampires.
Supplements for Porphyria
Beta-Carotene
Beta-carotene is a plant pigment that is converted into vitamin A in the body. It’s a powerful antioxidant that can help protect the skin from damage and reduce inflammation throughout the body. According to a study published in the Journal of the European Academy of Dermatology and Venereology, beta-carotene supplementation can help reduce the severity of porphyria-related skin damage. Feel free to visit our shop here at Bulksupplements.com to purchase beta-carotene supplements.
Magnesium
Magnesium is vital for porphyria patients as it helps to regulate the activity of the heme biosynthesis pathway. Additionally, magnesium has anti-inflammatory properties that help to reduce pain and inflammation in the body. It’s recommended that porphyria patients take a daily dose of 400 mg of magnesium.
Iron
One of the most common symptoms of porphyria is iron deficiency anemia. This is because the body uses iron to produce heme, which is lacking in people with porphyria. Iron supplements can help to raise iron levels and support the production of heme. It is important to talk to your doctor about the right dosage for you, as too much iron can be toxic.
Vitamin C
Vitamin C is an antioxidant that helps to prevent damage from free radicals in the body. It also helps to regulate the heme biosynthesis pathway and aids in the production of collagen, which is important for skin health. Porphyria patients should aim to take a daily dose of 500-1000 mg of vitamin C supplement.
Vitamin D
Many people with porphyria have low levels of vitamin D, which can worsen symptoms and increase the risk of bone loss and fractures. Vitamin D supplements can help to increase vitamin D levels and strengthen bones. Sunlight is also a natural source of vitamin D, so spending time outdoors can be beneficial for people with porphyria.
Coenzyme Q10
Coenzyme Q10 is a powerful antioxidant that helps to protect against cellular damage. People with porphyria may experience oxidative stress due to the build-up of certain substances in the body. Coenzyme Q10 supplements can help to reduce oxidative stress and improve energy levels.
Omega-3 Fatty Acids
Omega-3 fatty acids have anti-inflammatory properties that can help to reduce pain and inflammation in the body. They also help to improve brain function and heart health. Porphyria patients should aim to take a daily dose of 1000 mg of omega-3 fatty acids.
The Bottom Line
Porphyria isn’t just one disorder. It’s a word that describes at least 8 different conditions, mostly genetic, involving the accumulation of toxic porphyrins in the body. Porphyria can go unnoticed throughout a person’s lifetime or can suddenly a trigger severe, life-threatening situation. Researchers are working to understand how to better identify and treat porphyria. Some medications and therapies can help manage it, as can avoiding triggers that bring on an attack like sunlight, certain medications, and fasting.
Dealing with porphyria can be challenging, but there are a number of different supplements that can help support your body and reduce the impact of symptoms. From chloroquine to beta-carotene, iron to calcium, and vitamin D, there are many different options to explore. Just remember to talk to your doctor before starting any new supplement regimen, as they can advise you on the best course of action for your specific needs. With a little extra support, you can manage your porphyria symptoms and improve your overall quality of life.
These statements have not been evaluated by the Food and Drug Administration. These products are not intended to diagnose, treat, cure or prevent any disease