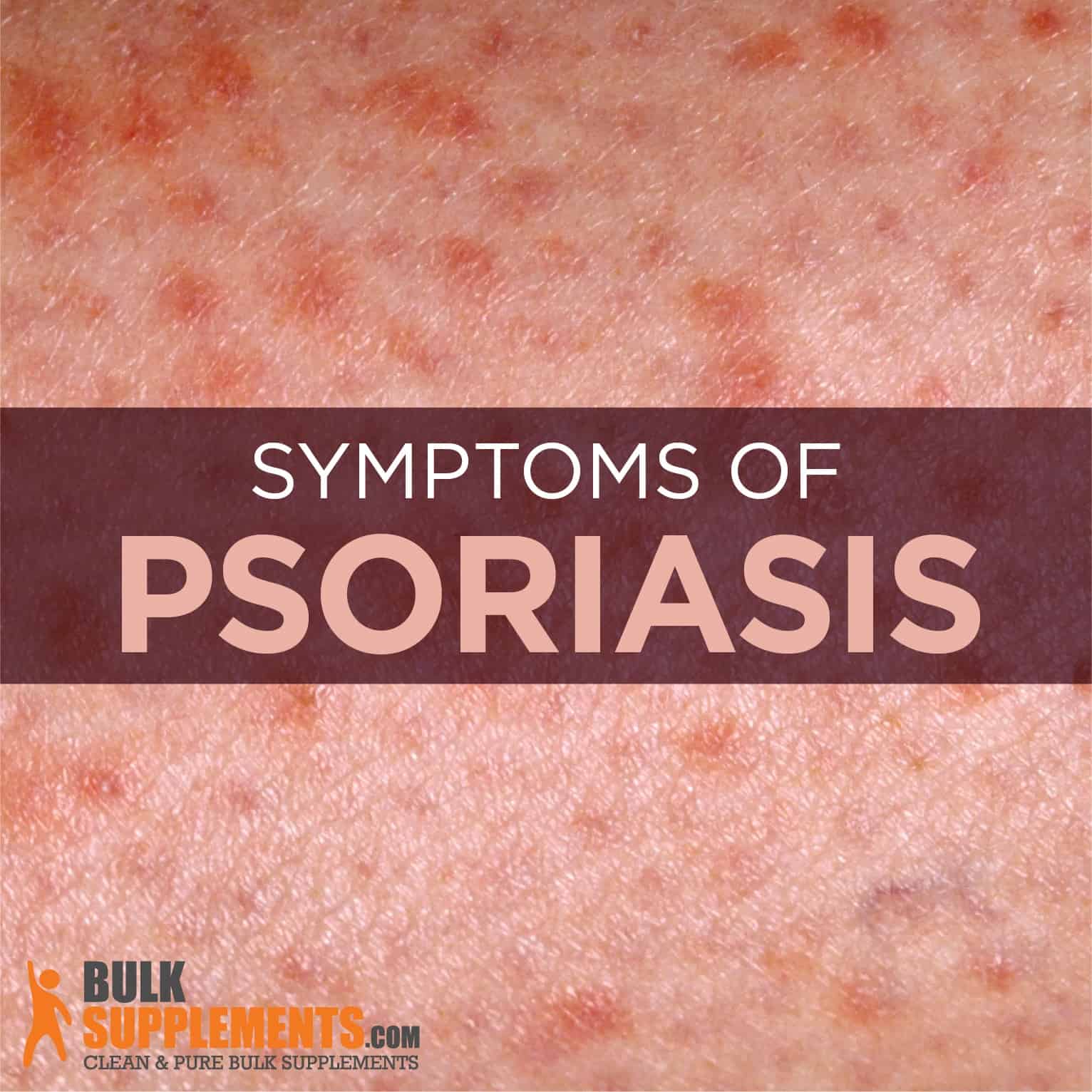
What is Psoriasis?
Psoriasis is an autoimmune skin disease that leads to a rapid build-up of skin cells. They grow abnormally fast — faster than your body can lose them — causing inflamed patches on the surface of the skin. Sometimes the patches itch, burn, or sting and, in some cases, they open up and begin to bleed. Usually, something triggers the lesions to flare. Understanding the cause of the triggers helps you control the health concern naturally.
Psoriasis may affect any part of your body, but it usually shows up on the elbows, knees or scalp. Symptoms vary depending on the type of psoriasis. It is also related to other conditions affecting the body and mind and spirit, such as cardiovascular disease, diabetes, and attitude. Attitude because the pain and itching are nerve-wracking with unsightly sores on your skin. (x)
Causes of Psoriasis
The cause of psoriasis is still puzzling to doctors and researchers alike. However, physicians now attribute two primary factors to the condition — genetics and the immune system.
Immune System
Psoriasis is an autoimmune condition, meaning the immune system mistakenly attacks itself and your body. In psoriasis, the immune system causes inflammation and rapid skin cell growth. T cells — a type of white blood cell — stimulate the immune system when they contact bacteria or viruses. T cells end up in the skin and attack skin cells, causing the body to produce new skin cells a lot more rapidly than expected. Your body produces new cells faster than it needs to and then transports them to the surface of the skin, where they begin to accumulate as dead cells. (x) (x)
Under normal conditions, skin cells take about a month to reproduce. But with psoriasis, the process may only take a few days. (x) New cells start their growth deep beneath the skin and gradually rise to the surface of the skin until they fall off as dead cells. But psoriasis causes new skin cells to reach the surface along with dead ones, and there is not enough time for cells to fall off before the new ones take their place. (x)
Genetics
Some people may have specific genes that increase their probability of developing psoriasis, though researchers haven’t found the particular genes. According to the National Psoriasis Foundation, at least 10 percent of people inherit the gene related to psoriasis. Still, only 2 to 3 percent end up developing the condition, so it’s a long shot but probable. (x) However, a twin study done in Australia discovered an 80 percent heritability for psoriasis, concluding that it is heritable. (x)
Psoriasis Triggers
Psoriasis flares in response to specific triggers. It appears that anything causing free radicals in your body triggers the health concern. Distinct cases respond to other triggers, but common ones include: (x) (x)
- Stress
- Skin injuries – cuts, burns, vaccinations
- Infections
- Medications
- Weather
- Alcohol and tobacco
- Allergies
- Psoriasis Symptoms
If psoriasis covers less than 3 percent of the body, the case is mild. If it covers between 3 and 10 percent, it is moderate, and a severe case covers over 10 percent. Symptoms depend on the type of psoriasis and usually vary among infected individuals. (x) (x)
The medical industry knows it is not contagious. Therefore, you cannot catch psoriasis by touching someone who has it, swimming in a pool with someone who has it or having sex with someone who has it. (x)
Different Kinds of Psoriasis
With different kinds of psoriasis, it’s essential to have the type identified to begin the appropriate treatment or remedy. Different psoriasis:
- Plaque Psoriasis
Plaque psoriasis is the most common type. Symptoms include thick, raised, red patches with white dead skin cell buildup. The plaques usually show up on the elbows, knees, scalp and lower back. Sometimes they itch, crack and bleed. (x) (x)
- Guttate Psoriasis
This type often begins in childhood, triggered by a strep infection. It shows up as tiny pink bumps on the torso, legs and arms, as well as the face, scalp and ears. It usually resolves without treatment after a few weeks or months and may not flare up again after it clears, but some people have it for life. (x) (x)
- Inverse Psoriasis
Inverse psoriasis flares where the skin touches skin — behind the knees, in the underarms or within the genitals — in smooth, sore red patches with white coating. Sometimes it accompanies other types of psoriasis at the same time. (x) (x)
- Pustular Psoriasis
Flaring usually occurs on the hands and feet. Pustular psoriasis causes red, swollen skin with bumps filled with pus. The skin is exceptionally sore and painful. (x) (x)
- Generalized Pustular Psoriasis
This type can be life threatening and spreads all over the skin, making it red, dry and tender. It develops into pus-filled bumps, which break open, and the skin dries out and peels. Then new bumps form and the process repeats itself. (x) (x)
- Erythrodermic Psoriasis
Erythrodermic psoriasis is incredibly aggressive but uncommon. It covers most of the body, making the skin look burnt with an intense itching or burning sensation. Other symptoms include fever, muscle weakness, and chills, which can develop into hypothermia. It is one of the most severe variants and can be life-threatening. (x) (x)
- Psoriatic Arthritis
People with psoriasis can develop psoriatic arthritis, which causes pain, swelling and stiffness in the joints because the immune system causes inflammation in the body. Most people notice it after they develop psoriasis, but some people have psoriatic arthritis without psoriasis. Other symptoms include fatigue, swollen fingers and toes, blurred vision and sensitivity to light. Psoriatic arthritis can cause permanent joint damage without treatment. (x) (x)

Other Conditions Caused by Psoriatic
People with psoriatic disease, including psoriatic arthritis, are more likely to develop other health conditions, including: (x)
- Cardiovascular disease
- Cancer – lymphoma, nonmelanoma skin cancer
- Crohn’s disease
- Diabetes
- Osteoporosis
However, studies suggest that treating psoriasis symptoms may reduce the risk of comorbid conditions. (x)
Psoriasis Treatment
Although there is no definite cure for psoriasis, there are treatments to help reduce the accumulation of skin cells and tone down inflammation. There are also treatments to remove plaques as well as relieve the itching and dryness. The type of treatment usually depends on several factors, including age, general health, the severity of the condition and the area it appears. There are three types of treatment: (x) (x) (x) (x)
- Topical Treatments
Usually, doctors will order topical treatments for patients first for mild or moderate cases. These treatments may effectively treat the condition, but it may take about six weeks for results. Topical treatments may include shampoo for scalp psoriasis, steroid creams or Vitamin D analog creams.
- Phototherapy
Phototherapy treats psoriasis using exposure to natural and artificial light that aims to slow down skin cell growth. Patients undergo these treatments if topical treatments are ineffective.
- Systemic Treatment
If the case is severe, doctors may prescribe systemic treatments that travel through the bloodstream. Medications are either biological — usually injections — or non-biological — usually tablets or capsules.
- Natural Remedies
You can combine them with other treatments. Natural remedies may also be effective in treating psoriasis, including: (x)
- Aloe vera to reduce redness and swelling
- Tea tree oil that acts as an antiseptic
- Apple cider vinegar to relieve itching
- Dead sea salts to remove plaque
- Mahonia, a plant that contributes to immune response as a homeopathic treatment (x)
Supplements for Psoriasis
Supplements can benefit your overall health and may also help treat some symptoms of psoriasis. Find out if pairing specific supplements with traditional treatments helps by first talking with your healthcare provider. You should speak with our doctor before starting any new supplement. Some supplements for psoriasis include:
- Omega-3-6-9 Softgels
Psoriasis and psoriatic arthritis patients are at a high risk of developing cardiovascular diseases. Omega-3-6-9 fatty acids help reduce the rate at which people contract heart diseases. (x) The recommended dosage is three soft gels once or twice per day.
- Milk Thistle Extract Powder
Also known as holy thistle, milk thistle is a natural antioxidant with anti-inflammatory qualities. It helps to ease psoriasis symptoms. It also prevents outbreaks by motivating the liver function and warding off T cell activation. (x) Take 250 mg daily as a dietary supplement.
- L-Glutamine Powder
Glutamine makes up more than half of the body’s skeletal muscle tissue and is a valuable energy source. It also promotes immune health. The suggested serving size is 1,000 mg up to three times per day on an empty stomach. Take the supplement either one hour before a meal or three hours after.
- Aloe Vera Extract Powder
Typically used as a topical gel, aloe vera reduces the scaling and redness of psoriasis when applied directly to the skin. (x) The extract powder promotes the immune system and circulatory health. Take 1,000 mg once a day with water.
- Vitamin A Palmitate Powder
It is a combination of palmitic acid and retinyl. Vitamin A palmitate has antioxidant properties and benefits skin health. (x) The recommended serving size is 30 mg once per day.
- Methylsulfonylmethane (MSM) Powder
MSM boosts skin health and supports healthy joints, which can be beneficial for psoriasis and psoriatic arthritis patients. One study reported improved pain from osteoarthritis. (x) The recommended serving size is 1000 to 1300 mg four times every day.
- Essential Oils
Apply with a carrier oil, like coconut or olive oils, with essential oils such as flora of Sicily, (x) lavender (x) and sandalwood. (x) The application of essential oils for your health is endless and worth investigating.
Where to Buy Supplements for Psoriasis?
You can purchase these powders and supplements for Psoriasis at BulkSupplements.com. The company is an industry-leading manufacturer and distributor of pure dietary supplements.
BulkSupplements.com is not just a consumer brand. It also supplies pure ingredients to other food and supplement brands to make their products. All products at BulkSupplements.com are manufactured and tested according to current and proper manufacturing practices.
Are you interested in trying any of these powders or supplements mentioned in this article as a possible solution to helping you with Psoriasis? Contact BulkSupplements.com to place an order today.
The Bottom Line
Psoriasis is an autoimmune disease in which the immune system mistakenly attacks healthy cells. In psoriasis, the immune system causes skin cells to grow faster than the body can get rid of them, resulting in lesions that build up on the surface of the skin. There are also genetic factors that increase the possibility of developing.
Symptoms vary depending on the type of condition, and usually, many factors can trigger them, such as stress, medication, allergies and infections. When your body experiences free radicals relating to oxidative stress, it’s essential to understand the value of antioxidants for this health condition. (x) Perhaps, a massive change in your lifestyle by committing to a healthier way of living.
There is no cure for psoriasis, but you can control it by topical treatments, phototherapy treatment, and medications. Natural remedies such as essential oils and supplements can help soothe symptoms and promote overall health.
These statements have not been evaluated by the Food and Drug Administration. These products are not intended to diagnose, treat, cure or prevent any disease.